COIN Investigators & Staff

COIN Affiliate
-
Evan Paul Carey, PhD, MS

- Title: COIN investigator and lead quantitative efforts for VACE
Assistant Professor, Department of Biostatistics and Informatics - Contact: evan.carey@va.gov
- Location: Denver
- University of Colorado webpage
Research Interests
See Dr. Carey's Dimensions profile that includes: publications, grants, datasets, patents and clinical trials
Dr. Carey focuses on evaluating new care initiatives or modalities in the VA, primarily focusing on the quantitative evaluation of the projects. He is the Co-Investigator on several mixed-methods projects. There is no particular clinical focus for these projects; the common theme is VA engagement in process improvement. The VA wants to understand the impact and outcome on Veterans or healthcare systems.

Dr. Carey follows the science and methods to achieve these aims. An approach to achieve this means creating an evaluation plan after the new project has started. His team attempts to determine the impact of the new care model in hospitals or clinics. Since the program is already underway and impacting Veterans or staff, they ask, "What would this target population look like if they never had this intervention?" Understanding and applying methods to this process through instrumental variable analysis lets us know if a new program has the hoped-for results.
Dr. Carey leads the quantitative analytic team for VA Collaborative Evaluation Center (VACE) and is the quantitative director for the University of Colorado Navigation Lab (NavLab). VACE is a highly collaborative VA "virtual center" composed of quantitative, qualitative, and mixed methods evaluation experts. The Navigation Lab's mission is to partner with UCHealth to perform rigorous and timely evaluation, implement and disseminate new knowledge and innovation, and engage relevant stakeholders within a Learning Health Systems (LHS) framework.
An example of this work is the VA's VIONE project. VIONE is a simple, user-friendly medication management methodology used to reduce polypharmacy and improve patient safety, comfort, and medication adherence consistent with high-reliability organizations and initially implemented in 2018-2019 throughout the VA. There are many potential benefits from increasing the Veterans' quality of life and saving the VA money. There are also potential downsides, like removing a medication that the Veteran needs. Dr. Carey's work is to determine if this program has the intended effect. Is it better for Veterans? Does it save money? Is there no unforeseen consequence?

To answer these questions, Dr. Carey and his team developed a mix-method study that works with but is independent of the VIONE project. The study will look at these questions specific to VIONE but can also explore system-wide questions related to health systems in general. Such as, does deprescribing medication have the desired outcome. The mixed-method part of this study is to ask the veterans what they think about the VIONE process. In the experience of the Veteran, is this leading to good outcomes?
A second domain Dr. Carey occupies is lead statistician for research projects. One such project is with Ann O'Hare in our Seattle lab, where she explores community care for Veterans with end-stage renal disease. The research uses a mixed-method study exploring the outcomes of community versus VA-based dialysis services. Community dialysis care was an outgrowth of the Veterans Choice Program that allows Veterans to choose care outside the VA when scheduling a VA appointment takes too long. Are the outcomes favorable to the Veteran? Is the Veteran seen in a timelier manner? Is there a cost-saving for the VA? How do Veterans feel about this change?

Dr. Carey's future work explores cutting-edge informatics techniques to enable the VA to become a proactive healthcare institution. Healthcare in the US is mainly reactive, especially in specialty care. The provision of services, especially specialty services, depends on a referral from a primary care clinician. Dr. Carey is interested in looking at models that proactively provide care based on what we know about a group and the needs that the population will or should need. He recently received an Implementation Research award from QUERI. to explore this idea related to chronic pain management. The goal of his project is to implement a precision population health dashboard in the context of chronic pain care among Veterans at the VA Eastern Colorado Healthcare System. Dr. Carey is being mentored by Joseph Frank, MD, and Michael Ho, MD.
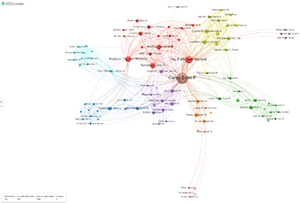
The following images visualize Dr. Carey's work. The word cloud is drawn from publication titles. The research collaboration map shows research relationships (click the image to enlarge):
| Publications | Grants |
|---|---|
| Clinical Research | Health Services |
| Health Services | Clinical Research |
| Cardiovascular | Cardiovascular |
| Heart Disease | Heart Disease |
| Patient Safety | Comparative Effectiveness Research |
| Clinical Trials and Supportive Activities | |
| Mental Health | |
| Behavioral and Social Science | |
| Prevention | |
| Pain Research |
Grants & Funding
Design and Implementation of an Informatics Tool Supporting Precision Population Health for Veterans Experiencing Chronic Pain
Role: Co-I
The goal of this study is to quantify the impact of contemporary VA community care policy on care and outcomes for Veterans with advanced kidney disease and identify opportunities to improve care coordination.
Applying Critical Race Theory to investigate the impact of COVID-19-related policy changes on racial/ethnic disparities in medication treatment for opioid use disorder
Role: Site-PI; PI's Emily Williams & Jessica Chen
With the rise in opioid use disorder (OUD) and overdose, racialized disparities in buprenorphine access and use are a significant concern nationally. Studies estimate that Black patients with OUD are 50-60% less likely to access buprenorphine than White patients, and similar disparities exist for Hispanic/Latinx patients.
COVID-19-related policy changes increased flexibility in providing buprenorphine and other effective medications for OUD over telehealth. They presented an unprecedented opportunity to examine the impacts of a structural intervention—relaxed MOUD restrictions—on disparities that result from structural racism and discrimination (SRD).
The proposed study, guided by Public Health Critical Race Praxis, will use data from the nation's largest provider of substance use care and quantitative and qualitative methods to examine the impact of these policy changes on racialized disparities for Black and Hispanic/Latinx patients to inform future policy and interventions to improve equitable care for OUD.
Funder: National Institute on Drug Abuse
NIH website
Expanding Veteran-to-Veteran Outreach & Group Support for Rural Veterans with Chronic Pain
Role: Co-I; PI: Joseph Frank
The goal of this project is to implement and evaluate a Veteran-facilitated peer support group for rural Veterans with chronic pain.
Improving Performance Evaluation of Clinicians to Support National Standards of Practice
Role: Site PI; PI: Jacob Doll
VA hospitals measure the performance of clinicians through systematic reviews of clinical care. These Ongoing Professional Practice Evaluations (OPPE) determine if clinicians are competent to continue VA practice. The current OPPE process is inefficient and does not have clear benefits for professional development or patient care.
A new VA mandate requires national standards of practice for all clinicians and methods to enforce these standards. With a focus on outpatient cardiology care, we propose to develop and test a novel two-tiered OPPE system:
1) Clinician assessment with electronic quality measures. Our research will establish the reliability of these measures and determine the best ways to measure clinicians.
2) Clinicians with substandard performance on quality measures will then encounter peer review. Our research will determine the best methods for peer review.
We will survey and interview clinicians to determine how current and proposed OPPE methods impact their practice and professional development.
Funder: Veterans Affairs
NIH website
VA Diffusion of Excellence: VA Polypharmacy and VIONE Evaluation
Role: PI
Description: This mixed methods evaluation will identify the impact of polypharmacy on Veteran outcomes, as well as de-prescribing efforts in the VA and the impact on Veteran outcomes.
Office of Rural Health: Oral Telemedicine Evaluation
Role: Quantitative Methodologist
Description: The goal of oral telemedicine is to provide all veterans across the nation with expert consultation from board certified specialists in oral pathology, oral medicine, and oral and maxillofacial surgery. This unique service is currently only available at the San Francisco VAHCS due to the scarcity of oral pathology and oral medicine specialists. The Evaluation will explore the implementation of the Oral Telemedicine using the Re-AIM framework and provide barriers and facilitators to enhance the implementation across VHA.
VA QUERI Partnered Evaluation Initiative (PEC 21-128): Evaluating the National Implementation of Virtual Interdisciplinary Pain Care Teams – TelePain
Role: Co-I; PI: Jessica Chen
Description: The proposed evaluation uses a rigorous prospective design to evaluate the impact of virtual interdisciplinary pain management teams (TelePain) on clinical outcomes for veterans, access to care, and costs to VA.
VA HSR / OCC: Understanding and Overcoming the Digital Divide in Specialty Care Following the onset of COVID-19
Role: PI
Description: The OCC_DigitalDivide project will leverage machine learning modeling to identify segments of the Veteran population who are at an increased risk of losing access to chronic pain care related outpatient care in the context of shifts to virtual care in the COVID-19 era.
Virtual Care QUERI Program: Implementing and Evaluating Technology Facilitated Clinical Interventions to Improve Access to High Quality Specialty Care for Rural Veterans.
Role: Co-I, rapid response team lead; PI: John Fortney
VA: Community Care for Veterans with Advanced Kidney Disease
Role: Co-I; PI: Ann O'Hare
We propose a mixed methods study to evaluate the impact of VA-financed community care for Veterans with advanced kidney disease. And to identify subgroups within this population most likely to benefit and be harmed by the receipt of nephrology care in the community.
These patients comprise a high-cost, high-needs segment of the Veteran population facing a critical health and care transition (onset of end-stage renal disease).
The work we propose is highly relevant to the VA mission (it will directly address three VA HSR priority areas), timely (the VA MISSION Act recently received strong bipartisan support in both the House and the Senate), and will directly inform evolving VA policy around the provision of community care for Veterans.
Funder: Veterans Affairs
NIH website
Publications of note:
— Implications of Cross-System Use Among US Veterans With Advanced Kidney Disease in the Era of the MISSION Act
FLOW3 Partnered Evaluation
Role: Co-I; PIs: Chelsea Leonard, Michael Ho, and Jeffrey Heckman, DO
Description: The goal of this study is to quantify the impact of contemporary VA community care policy on care and outcomes for Veterans with advanced kidney disease and identify opportunities to improve care coordination.
VA Office of Rural Health: Project Atlas Rural Telehealth National Evaluation & Review (PARTNER)
Role: Quantitative Methodologist
VA HSR: Denver-Seattle Center of Innovation for Veteran-centric and Value driven care
Role: Methodologist
Description: This is a VA HSR Center of Innovation (COIN) funded to conduct outstanding health services research that promotes Veteran-centered and value-driven care, generate and disseminate knowledge that contributes to the well-being of Veterans, partner with VA policy and operational leaders to implement research findings into clinical care, and train the next generation of health services researchers and leaders.
Recent Publications
2024
Javier SJ, Carey EP, Gunzburger E, Chen HP, Zeliadt SB, Williams EC, Chen JA. Pain Care Disparities and the Use of Virtual Care Among Racial-Ethnic Minority Groups During COVID-19. J Gen Intern Med. 2024 Jan 22. doi: 10.1007/s11606-023-08473-0. Epub ahead of print.
PMID: 38252245.
Learn more about this publication on Dimensions
2023
Mistry N, Richardson V, Carey E, Porter S, Pincus S, Novins-Montague S, Elmer M, Lin CT, Ho PM, Anstett T. General improvements versus interruptive or non-interruptive alerts in the blood order set: study protocol for a randomized control trial to improve packed red blood cell utilization. Trials. 2023 May 8;24(1):314. doi: 10.1186/s13063-023-07319-8. PMCID: PMC10165805.
PMID: 37158929.
Learn more about this publication on Dimensions
Carey E, Chen HP, Baker D, Blankenhorn R, Munro S. Non-Ventilator Associated Hospital Acquired Pneumonia (NV-HAP) Risk Among Hospitalized Veterans Before and During the COVID-19 Pandemic. Am J Infect Control. 2023 Jan 2:S0196-6553(22)00888-4. doi: 10.1016/j.ajic.2022.12.012. Epub ahead of print. PMCID: PMC9807267.
PMID: 36603808.
Learn more about this publication on Dimensions
2022
Smilowitz NR, Carey EP, Shah B, Hartigan PM, Plomondon ME, Maron DJ, Maddox TM, Spertus JA, Mancini GBJ, Chaitman BR, Weintraub WS, Sedlis SP, Boden WE; COURAGE Trial Investigators and VA CART CL. Comparison of Characteristics and Outcomes of Veterans With Stable Ischemic Heart Disease Enrolled in the COURAGE Trial Versus the Veterans Affairs Clinical Assessment, Reporting, and Tracking Program. Am J Cardiol. 2022 Jul 30:S0002-9149(22)00699-3. doi: 10.1016/j.amjcard.2022.06.049. Epub ahead of print.
PMID: 35918234.
Learn more about this publication on Dimensions
O'Hare AM, Butler CR, Laundry RJ, Showalter W, Todd-Stenberg J, Green P, Hebert PL, Wang V, Taylor JS, Van Eijk M, Matthews KL, Crowley ST, Carey E. Implications of Cross-System Use Among US Veterans With Advanced Kidney Disease in the Era of the MISSION Act: A Qualitative Study of Health Care Records. JAMA Intern Med. 2022 May 16. doi: 10.1001/jamainternmed.2022.1379. Epub ahead of print.
PMID: 35576068.
Learn more about this publication on Dimensions
Fortney JC, Carey EP, Rajan S, Rise PJ, Gunzburger EC, Felker BL. A Comparison of Patient-Reported Mental Health Outcomes for the Department of Veterans Affairs' Regional Telehealth and Community Care Programs. Health Serv Res. 2022 Apr 25. doi: 10.1111/1475-6773.13993. Epub ahead of print.
PMID: 35467011
Learn more about this publication on Dimensions
Horn CB, O'Malley JF, Carey EP, Culhane JT. Hospital-Acquired Condition Rate of Admitting Facility Does Not Predict Mortality in Traumatically Injured Patients. Cureus. 2022 Apr 7;14(4):e23908. doi: 10.7759/cureus.23908. PMCID: PMC9088883.
PMID: 35547464
Learn more about this publication on Dimensions
Carey E, Chen HP, Baker D, Blankenhorn R, Vega RJ, Ho M, Munro S. The Association between Non-Ventilator Associated Hospital Acquired Pneumonia and Patient Outcomes Among U.S. Veterans. Am J Infect Control. 2022 Feb 26:S0196-6553(22)00102-X. doi: 10.1016/j.ajic.2022.02.023. Epub ahead of print.
PMID: 35231564.
Learn more about this publication on Dimensions
Seal KH, Bertenthal D, Carey E, Grunfeld C, Bikle DD, Lu CM. Association of Vitamin D Status and COVID-19-Related Hospitalization and Mortality. J Gen Intern Med. 2022 Jan 1:1–9. doi: 10.1007/s11606-021-07170-0. Epub ahead of print. PMCID: PMC8723909.
PMID: 34981368.
Learn more about this publication on Dimensions
2021
Munro SC, Baker D, Giuliano KK, Sullivan SC, Haber J, Jones BE, Crist MB, Nelson RE, Carey E, Lounsbury O, Lucatorto M, Miller R, Pauley B, Klompas M. Nonventilator hospital-acquired pneumonia: A call to action. Infect Control Hosp Epidemiol. 2021 Aug;42(8):991-996. doi: 10.1017/ice.2021.239. Epub 2021 Jun 9.
PMID: 34103108.
Carey E, Blankenhorn R, Chen P, Munro S. Non-Ventilator Associated Hospital Acquired Pneumonia Incidence and Health Outcomes Among U.S. Veterans from 2016-2020. Am J Infect Control. 2021 Jun 8:S0196-6553(21)00399-0. doi: 10.1016/j.ajic.2021.06.001. Epub ahead of print.
PMID: 34116083.
Griffith MF, Chen HP, Bekelman DB, Feemster LC, Spece LJ, Donovan LM, Au DH, Carey EP. Comorbid Anxiety and Depression, Though Underdiagnosed, Are Not Associated with High Rates of Low-Value Care in Patients with Chronic Obstructive Pulmonary Disease. Ann Am Thorac Soc. 2021 Mar;18(3):442-451. doi: 10.1513/AnnalsATS.201912-877OC. PMCID: PMC7919148.
PMID: 33306930.
2020
Frank JW, Carey E, Nolan C, Hale A, Nugent S, Krebs EE. Association Between Opioid Dose Reduction Against Patients' Wishes and Change in Pain Severity. J Gen Intern Med. 2020 Dec;35(Suppl 3):910-917. doi: 10.1007/s11606-020-06294-z. Epub 2020 Nov 3. PMCID: PMC7728978.
PMID: 33145690.
2019
Donovan LM, Coggeshall SS, Spece LJ, Griffith MF, Palen BN, Parsons EC, Todd-Stenberg JA, Glorioso TJ, Carey EP, Feemster LC, Zeliadt SB, Kirsh S, Au DH. Use of In-Laboratory Sleep Studies in the Veterans Health Administration and Community Care. Am J Respir Crit Care Med. 2019 Sep 15;200(6):779-782. doi: 10.1164/rccm.201902-0313LE. PMCID: PMC7330508.
PMID: 31206308.
Frank JW, Carey E, Nolan C, Kerns RD, Sandbrink F, Gallagher R, Ho PM. Increased Nonopioid Chronic Pain Treatment in the Veterans Health Administration, 2010-2016. Pain Med. 2019 May 1;20(5):869-877. doi: 10.1093/pm/pny149.
PMID: 30137520.